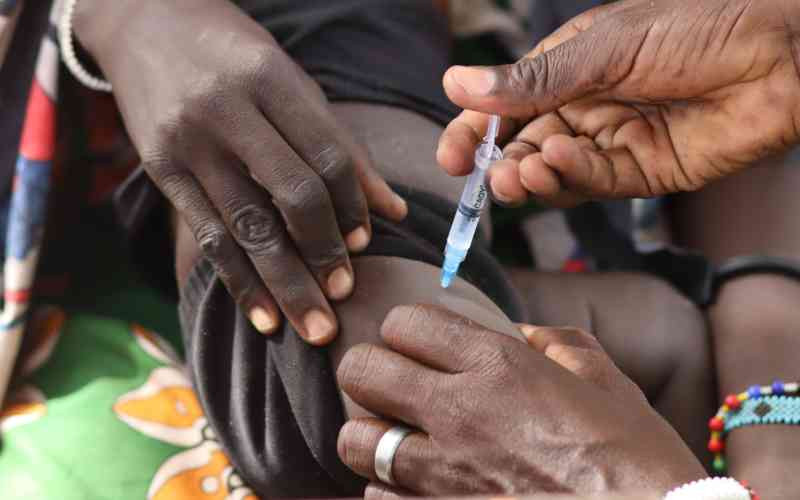
KENTTEC’s zoologist Nancy Miron explains to a farmer Hassan Ibrahim how a biconical tsetse fly trap works to prevent the spread of sleeping sickness in Kina, isiolo county, on March 5, 2017. [File, Standard]
The small, dusty village of Bagata feels a familiar chill run through it every time the sun dips below the horizon, but it isn’t just the evening air. It is the creeping shadow of Ndoki, the "sleeping sickness," a silent assassin that has haunted generations. For Mama Adisa, the fear became a brutal reality when her vibrant 14-year-old grandson, Kito (not his real name), began to change. His usual boundless energy faded into a lethargy that deepened with each passing day. The playful twinkle in his eyes dulled, replaced by a vacant stare. “He would fall asleep unexpectedly, sometimes even mid-sentence,” his mother narrates, adding that the tremors began soon after, violent shakes that wracked his small frame. Adisa knew the signs. She had seen Ndoki claim too many, slowly stealing their loved ones until they slept forever.
"It was like watching a part of him disappear each day," Adisa recounts, her voice still laced with the pain of those memories. "We prayed. We tried traditional medicines. But the disease, it always won. The doctors in the past, they had needles, and the medicine made people sicker before they got better. Sometimes, it killed them too."
Kito's diagnosis confirmed their worst fears: Trypanosoma brucei gambiense, the most common form of human African trypanosomiasis, or sleeping sickness.
Kito’s case is not isolated. Sleeping sickness—scientifically known as human African trypanosomiasis and most commonly caused by Trypanosoma brucei gambiense—has long been one of the most neglected tropical diseases affecting rural populations in sub-Saharan Africa. But today, a new chapter of hope is beginning to emerge.
For decades, treatment options were limited and often frightening. Older therapies required painful injections and complex hospital procedures. Many patients became sicker before they began to recover, and in some cases, the treatment itself carried serious risks. These realities left many communities fearful of both the disease and the treatment.
A groundbreaking new treatment called Acoziborole has recently been approved. The drug has been developed by the Drugs for Neglected Diseases initiative (DNDi) in partnership with Sanofi. Unlike older treatments that required hospital stays and multiple injections, Acoziborole is administered as a single oral tablet, making it far simpler to deliver in remote and resource-limited settings.
- Researchers find malaria's weak point, offer hope for world children
- Explainer: Nipah virus: What is it?
- Nipah virus revives pandemic fears, as Kenya risk termed low
- Guarding the gains: Africa moves to tackle rising HIV drug resistance
Keep Reading
As countries prepare to roll out the treatment, health experts believe it could significantly transform the fight against sleeping sickness. Patients who once faced long and painful treatment processes may soon have access to a safer and more accessible option.
For communities that have lived for decades under the shadow of Ndoki, the approval of this drug signals something powerful: the possibility that future generations will confront the disease with better tools, renewed hope, and a real chance to defeat it.
The World Health Organisation (WHO) officially validated Kenya as having eliminated Human African Trypanosomiasis (HAT), or sleeping sickness, as a public health problem in August 2025. This makes Kenya the tenth country to achieve this milestone. This elimination was the result of consistent control activities over many years, including strengthening surveillance in 12 health facilities across six historically endemic counties, equipping them with diagnostic tools, and training personnel. Kenya also actively monitors tsetse flies and animal trypanosomiasis. But the Democratic Republic of the Congo (DRC), which accounts for more than 70 per cent of all reported Human African Trypanosomiasis (HAT or sleeping sickness) cases in sub-Saharan Africa, is yet to achieve this ground-breaking milestone. The highest burden is concentrated in remote, rural areas of the former provinces of Bandundu, Equateur, and Province Orientale.
However, there could be some light at the end of the tunnel after the European Medicines Agency (EMA) has issued a positive opinion for Acoziborole Winthrop, a new three-tablet, single-dose oral treatment for Trypanosoma brucei gambiense, the most common form of sleeping sickness. This development, a collaborative effort by DNDi (Drugs for Neglected Diseases initiative) and Sanofi, aims to simplify treatment and support the World Health Organisation’s (WHO) goal of eliminating the disease by 2030.
On February 27, 2026, the EMA’s Committee for Medicinal Products for Human Use (CHMP) recommended acoziborole for treating both early and advanced stages of gambiense sleeping sickness in adults and adolescents aged 12 and above, weighing at least 40 kilograms. This endorsement, part of the EU-M4all procedure for high-priority medicines, confirms the treatment meets EU standards. It is expected to expedite regulatory approval in endemic countries, starting with the Democratic Republic of Congo (DRC), and will inform revisions to the WHO sleeping sickness treatment guidelines, enhancing access across Central and West Africa.
Historically, sleeping sickness treatment posed considerable challenges. Two decades ago, advanced-stage patients relied on an arsenic-based injection that carried a five per cent mortality risk. While lethal if untreated, the arsenic regimen was often the only available option. Over time, DNDi and Sanofi, in partnership with endemic nations, introduced improved treatments. These included the NECT (nifurtimox-eflornithine combination therapy) injectable in 2009, and fexinidazole, the first oral treatment requiring a 10-day course, in 2018. Acoziborole is the outcome of this sustained research and development, providing a more streamlined approach.
"The development of acoziborole and today’s positive scientific opinion is a victory for Africa-led science," declared Dr Erick Miaka, Director of the DRC’s national sleeping sickness control programme. He highlighted the pivotal role of "African doctors and researchers who conducted cutting-edge pharmaceutical research in some of the most remote and difficult-to-reach areas on the continent." According to him, this isn't just medicine developed for Africa; it's medicine developed with Africa.
These therapeutic advancements have markedly reduced disease incidence. In 1998, approximately 40,000 cases of gambiense sleeping sickness were reported, with an estimated 300,000 undiagnosed. By 2024, reported cases had decreased to under 600. The simplified, one-day oral treatment is expected to further accelerate this decline. As humans are the sole reservoir for the parasite, rapid and accessible treatment is critical for preventing transmission and achieving elimination.
Sanofi has committed to donating Acoziborole Winthrop to the WHO through its philanthropic entity, Foundation S – The Sanofi Collective. This ensures the medicine will be available free of charge to patients. Additionally, studies are ongoing in the DRC and Guinea to evaluate acoziborole's efficacy in children aged 1 to 14.
The positive opinion for acoziborole signifies a substantial step forward in combating sleeping sickness. It reflects sustained investment and collaborative models in neglected disease research, enabling simplified test-and-treat strategies that could lead to the elimination of gambiense sleeping sickness by 2030.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.